Prenatal Screening | Vibepedia
Prenatal screening encompasses a suite of medical tests designed to identify potential birth defects and genetic disorders in a fetus before birth. These…
Contents
Overview
Prenatal screening encompasses a suite of medical tests designed to identify potential birth defects and genetic disorders in a fetus before birth. These methods range from non-invasive blood tests and ultrasounds to more definitive diagnostic procedures like amniocentesis and chorionic villus sampling (CVS). The goal is to provide expectant parents with crucial information about their baby's health, enabling informed decisions regarding pregnancy management, delivery, and postnatal care. While screening tests offer probabilities, diagnostic tests provide definitive diagnoses for conditions such as Down syndrome, cystic fibrosis, and neural tube defects. The field has seen rapid advancements, particularly with the advent of non-invasive prenatal testing (NIPT), which analyzes fetal DNA fragments in maternal blood, significantly reducing the need for invasive procedures. However, ethical considerations surrounding genetic information, potential for discrimination, and the psychological impact on families remain central to the ongoing discourse.
🎵 Origins & History
The quest to understand fetal health predates modern medicine, with early attempts at divination and observation. The development of ultrasound in the 1950s and 60s by pioneers like Ian Donald revolutionized obstetric imaging, allowing for visual inspection of the fetus. Simultaneously, advances in cytogenetics enabled the analysis of fetal chromosomes. Amniocentesis, a diagnostic procedure involving the withdrawal of amniotic fluid, offered direct genetic analysis. The subsequent development of chorionic villus sampling (CVS) provided an earlier diagnostic option. These diagnostic tools paved the way for screening tests that could identify pregnancies at higher risk, guiding decisions about whether to proceed with invasive diagnostic procedures. The early 21st century marked a seismic shift with the introduction of non-invasive prenatal testing (NIPT), a testament to the accelerating pace of biotechnology innovation.
⚙️ How It Works
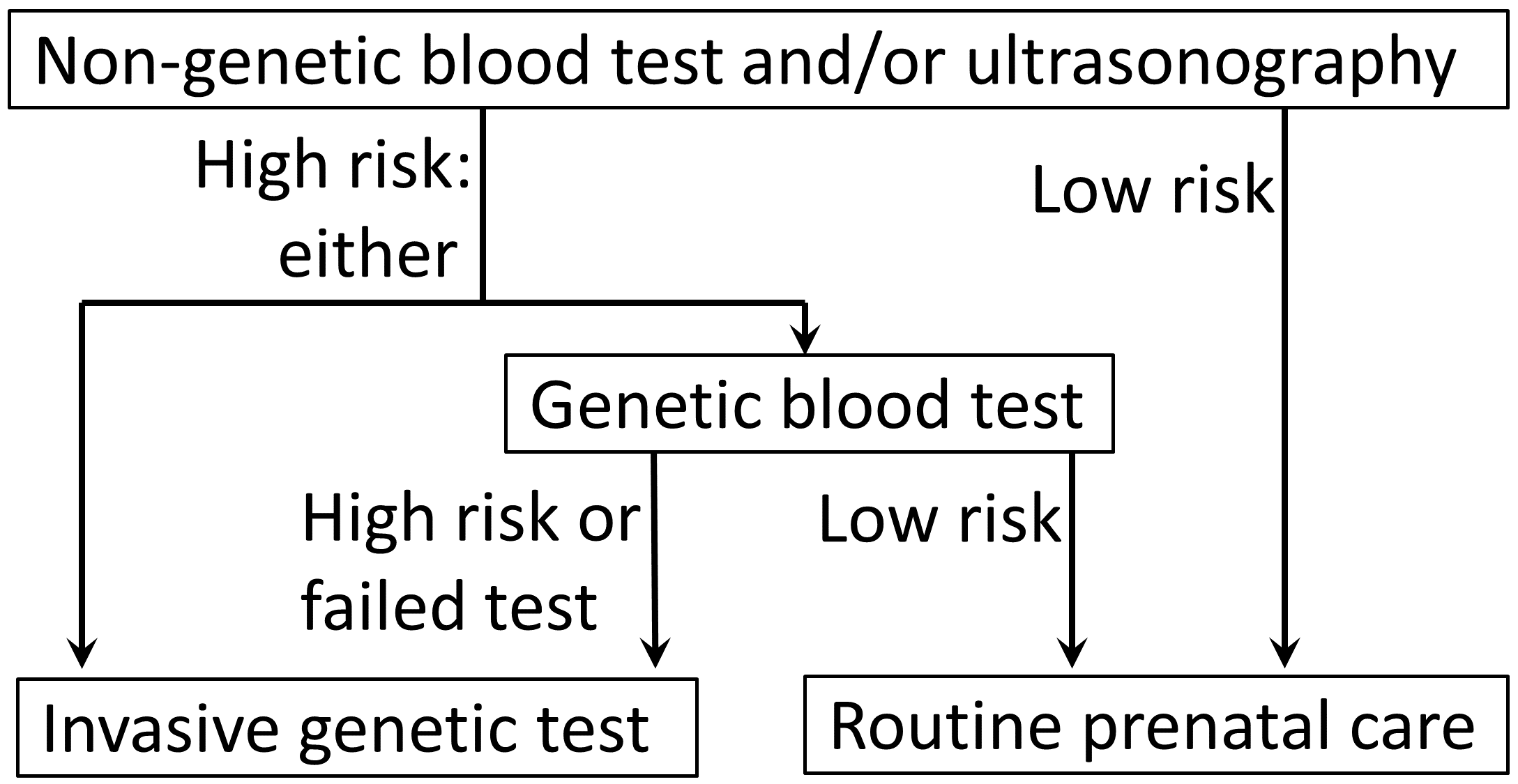
Prenatal screening employs a multi-pronged approach, often beginning with maternal serum screening (MSS) during the first and second trimesters. These blood tests measure levels of specific proteins and hormones, such as PAPP-A and AFP, which can indicate an increased risk for certain chromosomal abnormalities like Down syndrome (Trisomy 21), Trisomy 18, and neural tube defects like spina bifida. These results are often combined with maternal age and ultrasound findings, particularly nuchal translucency measurements, to calculate a risk score. For a definitive diagnosis, invasive procedures like amniocentesis (sampling amniotic fluid) or CVS (sampling placental tissue) are performed, allowing for direct chromosomal and genetic analysis. The most recent innovation, NIPT, analyzes cell-free fetal DNA circulating in the maternal bloodstream, offering high accuracy for common aneuploidies with minimal risk.
📊 Key Facts & Numbers
Globally, approximately 10-15% of pregnancies are affected by birth defects, a figure that underscores the significance of prenatal screening. In the United States alone, over 1 million babies are born with birth defects annually. First-trimester screening, combining ultrasound and maternal blood tests, can detect about 85-90% of Down syndrome cases. NIPT, now utilized in over 50% of pregnancies in some high-income countries, boasts detection rates for Trisomy 21 exceeding 99% with a false-positive rate below 1%. Invasive diagnostic procedures like amniocentesis carry a miscarriage risk of approximately 0.1-0.3%. The market for prenatal screening tests is substantial, projected to reach over $5 billion globally by 2027, driven by technological advancements and increasing parental demand for genetic information.
👥 Key People & Organizations
Key figures in the development of prenatal screening include Ian Donald, a Scottish obstetrician credited with pioneering diagnostic ultrasound in the 1950s. Mary-Claire King, a renowned geneticist, has made significant contributions to understanding human genetics, including work relevant to inherited diseases. Organizations like the American College of Obstetricians and Gynecologists (ACOG) and the World Health Organization (WHO) establish guidelines and recommendations for prenatal care and screening. Leading companies in the diagnostic sector, such as Sequenom (now part of Medtronic), Illumina, and Myriad Genetics, have been instrumental in developing and commercializing advanced screening technologies, including NIPT.
🌍 Cultural Impact & Influence
Prenatal screening has profoundly reshaped societal perceptions of pregnancy and disability. It has empowered expectant parents with knowledge, enabling them to prepare for potential challenges or make deeply personal decisions about pregnancy continuation. The widespread availability of screening has also contributed to a cultural shift, where the expectation of a 'perfect' baby can inadvertently place pressure on families. For conditions like Down syndrome, screening has been linked to declining birth rates, sparking intense ethical debates. Furthermore, the information gleaned from prenatal tests can influence obstetric management, allowing for specialized care during pregnancy and delivery for infants identified with specific conditions, thereby improving neonatal outcomes. The cultural resonance of these tests is undeniable, often becoming a rite of passage in modern pregnancy.
⚡ Current State & Latest Developments
The landscape of prenatal screening is in constant flux, driven by rapid advancements in genomic sequencing and bioinformatics. The integration of whole-genome sequencing into prenatal diagnostics is on the horizon, promising the detection of a wider array of genetic conditions. Efforts are underway to expand NIPT to screen for microdeletions and other rarer genetic anomalies, further enhancing its utility. Regulatory bodies like the U.S. Food and Drug Administration (FDA) are grappling with how to appropriately regulate direct-to-consumer genetic tests and ensure the accuracy and ethical use of NIPT. The ongoing development of artificial intelligence in analyzing complex genetic data and ultrasound images also promises to refine screening accuracy and efficiency in the coming years.
🤔 Controversies & Debates
The ethical implications of prenatal screening are a significant point of contention. Critics raise concerns about the potential for eugenics, arguing that widespread screening could devalue the lives of individuals with disabilities. The psychological burden on expectant parents, who must grapple with probabilistic results and potentially life-altering decisions, is also a major consideration. Questions surrounding informed consent, genetic privacy, and the potential for discrimination based on genetic information are paramount. Furthermore, disparities in access to advanced screening technologies, particularly NIPT, raise concerns about equity in healthcare, with lower-income populations and certain ethnic minorities often having less access to these cutting-edge diagnostics.
🔮 Future Outlook & Predictions
The future of prenatal screening points towards increasingly comprehensive and accessible genetic information. We can anticipate NIPT evolving to detect a broader spectrum of genetic conditions, including single-gene disorders, with even greater accuracy and at earlier gestational ages. The integration of polygenic risk scores may allow for the assessment of predisposition to common complex diseases. As technology advances, the cost of these tests is likely to decrease, potentially making them universally accessible. However, this expansion will undoubtedly intensify the ethical debates surrounding genetic determinism, reproductive autonomy, and the societal definition of 'normal' or 'healthy'. The challenge will be to harness these powerful technologies responsibly, ensuring they serve to support families rather than dictate reproductive choices.
💡 Practical Applications
Prenatal screening has direct practical applications in guiding obstetric care and preparing families for a child's specific needs. For instance, identifying congenital heart disease prenatally can allow for specialized cardiac care immediately after birth. Knowledge of conditions like hemophilia or sickle cell anemia enables parents to connect with support groups and medical specialists early on. Screening for gestational diabetes in the mother directly impacts dietary recommendations and monitoring during pregnancy. For conditions like spina bifida,
Key Facts
- Category
- science
- Type
- topic